Skin Cancer
Get Experienced Care for Cancers of the Skin or Pre-Cancerous Lesions in Marco Island and Naples, Florida
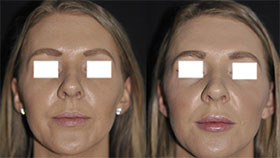
At Skin Wellness Physicians in Naples, Florida, skin cancer diagnosis and treatment are available for any patients who think they have any symptoms of the disease or who notice any unusual or worrying skin changes. The board-certified dermatologists at Skin Wellness Physicians work tirelessly to identify not just the nature and extent of a patient's cancer, but also the treatment that will provide the best chance at a cure, while preserving as much healthy tissue as possible.
Contact Skin Wellness Physicians if you would like more information on the diagnosis and treatment of skin cancer in Naples and Marco Island, FL. Request a consultation by sending a message online or calling (239) 732-0044.
What Is Skin Cancer?
While just about everyone knows that the sun is related to skin cancer (a fact highly familiar to those of us in Florida), we do still hear the question worth answering: What is skin cancer caused by? This cancer is an abnormal growth of skin cells that often forms on areas that are frequently exposed to the sun, but it may also develop on areas that aren’t usually sun exposed.
This disease is the most common type of human cancer and occurs when there’s a transformation in normal cells that causes them to grow and multiple abnormally. Rapidly dividing cells can form a mass called a tumor, which may remain contained or become malignant, which means the cancerous cells spread and invade neighboring tissues, organs, and systems.
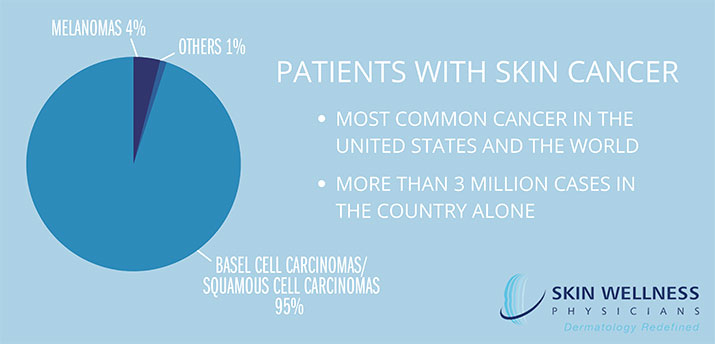
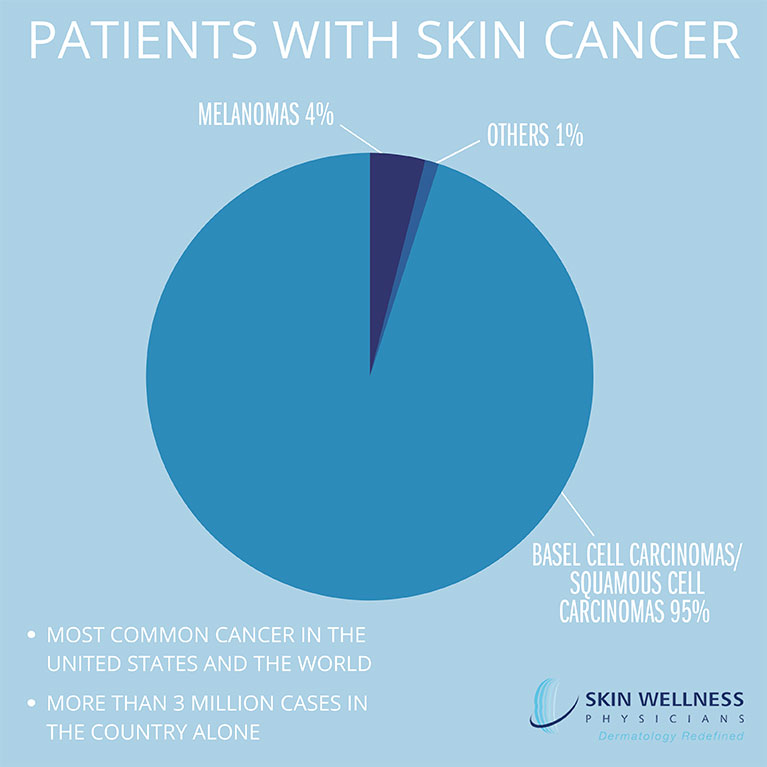
Skin cancer is a condition commonly seen by our providers. In fact, skin cancer is the most common cancer in the United States and the world, with more than 3 million cases in the country alone. Approximately 95 percent of skin cancers in the U.S. are one of two types: basal cell carcinomas and squamous cell carcinomas. Melanoma makes up about 4 percent of skin cancers in the United States, but is the cause of about three-quarters of all skin cancer deaths. The remaining 1 percent is made up of a large number of skin cancers that all occur very rarely.
What Are the Different Types of Skin Cancer?
What are the different types of skin cancer and how do they differ? Which type of skin cancer is most likely to be fatal? How does basal cell carcinoma (BCC) differ from squamous cell carcinoma (SCC)?
These are some of the most common questions we get asked about the disease. There are three main types of cancers that dermatologists will typically look for during a skin exam or skin check:
Basal Cell Carcinoma
Basal cell carcinomas are the most common skin cancer and originate from hair follicles. That is why we do not find basal cell cancers on the palms or soles, where we do not have hair follicles.
Basal cell carcinomas rarely ever cause death or travel to the lymph nodes, but they can cause significant local destruction, mutilation, and functional deficits if they are allowed to invade local anatomic structures such as the eye, nose, ears, or nerves, resulting in facial paralysis. These skin cancers are slow growing, but grow faster the larger they are.
Squamous Cell Carcinoma
Squamous cell carcinomas come from the epidermal lining of the skin. Therefore, we can find SCC on any skin lining, even the palms and soles. Squamous cell carcinomas can arise from a precursor or "pre-cancer" called actinic keratoses (AK) or from out of nowhere (de novo). This is why dermatologists place such an emphasis on treating the rough spots on patients' sun-exposed locations in order to prevent them from progressing to cancer. Squamous cell carcinomas are more dangerous than basal cell carcinomas in that these skin cancers can metastasize to the lymph nodes, brain, lungs, or liver, ultimately causing death. While this is a rare event, it is important to address squamous cell carcinomas early when they are easier to treat and carry a lower risk of metastasis to other organs.
Melanoma
Melanoma is the most dangerous or serious type of the three most common skin cancers. This form of cancer develops in the melanocytes, which are cells that produce melanin or pigment to give skin its color. They can develop anywhere on the body but are common on sun exposed areas. Melanoma grows rapidly and can quickly metastasize, spreading to other areas of the body.
How Is Skin Cancer Diagnosed?
How do doctors test for skin cancer? How is skin cancer identified? What are skin exams for cancer?
Diagnosis of cancerous cells in the skin will involve a dermatologist examining your skin and sometimes removing a sample of a suspicious lesion for lab testing to confirm the diagnosis and identify what type of skin cancer you have. Screenings at home and with your dermatologist are vital to help you catch any signs of the disease as early as possible, but it’s important to recognize that at-home checks are not a replacement for professional ones. A skin exam or screening allows us to check for unusual changes in the skin or signs of skin cancer. If you have a high risk for this cancer or a history of the disease, you will need to get skin exams more frequently.
Want more advice on diagnosing and treating skin cancer in the Naples and Marco Island area? Schedule a consultation at Skin Wellness Physicians by sending a message online or calling (239) 732-0044..
How Is Skin Cancer Treated?
“Can you recover from skin cancer?” This is one of the most pressing concerns many individuals will undoubtably have. There are numerous treatments available. The best solution will depend on factors such as the type, stage, severity, size, and location of the skin cancer tumor. There is no one-size-fits-all approach for this disease, so an appropriate and patient-specific treatment plan should be discussed with your dermatologist. Ultimately, treatments for cancers of the skin can broadly be thought of as existing in two categories: non-blinded and blinded.
NON-BLINDED
"Non-blinded" skin cancer treatments refer to the careful examination of the margins of the tissue to ensure that the cancer has been removed. There are only two procedures that can be considered "non-blinded." The first and most effective of all treatments is Mohs surgery.
This method, developed by the late Dr. Frederich Mohs, uses a technique where 100 percent of the surgical margin can be evaluated. In fact, this is the only technique where the entire surgical margin is evaluated. All other treatments either do not evaluate the margins or evaluate a lesser amount. Mohs surgery is reserved for skin cancers that occur on certain body locations, are of a certain size, carry some increased risk based on their appearance under the microscope, or involve other extenuating circumstances (including, but not limited to, the patient being young, immunosuppression, recurrence, appearing in a burn scar, etc.). The approach allows the surgeon to take less tissue than what would normally be required because of the ability to evaluate 100 percent of the margin and therefore conserve more of the patient's skin than other procedures. The processing of the tissue can take about an hour, which can often cause significant wait times in the office. By definition, this technique refers to the surgeon acting as both the surgeon and the pathologist.
Mohs surgery offers the highest cure rates of any other treatment: 95 to 99 percent, when done by a Mohs College fellowship-trained surgeon. All clinical trials validating these cure rates were done studying Mohs College fellowship-trained members, who can be found here. If a surgeon is not found on this site, they have not done a one-year dedicated fellowship.
Once the skin cancer is removed, the most cosmetically acceptable reconstruction is performed. Mohs College fellowship-trained surgeons have undergone an intensive one-year training not only learning the surgical removal and evaluation of skin cancer, but also learning and performing the most advanced reconstruction techniques available. Furthermore, Mohs College members are required to frequently attend national conferences in order to maintain their fund of knowledge on the most cutting edge surgical removal and repair techniques.
In very rare instances, collaboration with a non-dermatologist surgeon, such as a plastic surgeon or ENT, is recommended.
The other non-blinded treatment option is simple excision, which involves taking out the tissue in a non-Mohs technique. This is appropriate and often used for smaller skin cancers on the trunk and extremities. Under these circumstances, the treatment offers high cure rates with good cosmetic outcomes. While the margins are evaluated, only a fraction of the margins are evaluated when compared to Mohs.
None of the margins are evaluated with "blinded" treatments.
Meet our Dermatologists

At Skin Wellness Physicians, our dermatologists are board certified and thoroughly experienced in a range of medical and cosmetic treatments.





BLINDED
"Blinded" skin cancer treatments refer to those that do not check the margins of a skin cancer lesion, such as radiation therapy, electrodessication and curettage (ED&C), photodynamic therapy, and topical therapies. The treatments are based on clinical trials that determine how much or how little should be treated based on multiple factors. Most treatments are blinded. A very good treatment with high cure rates in some instances is radiation therapy. There are several different types of radiation treatments that vary in cost, treatment number, and side effects. If radiation therapy is recommended for your skin cancer, the details of these options will be discussed with your radiation oncologist.
"Scraping and burning"—known professionally as electrodessication and curettage (ED&C)—is a good option in some circumstances, but can often lead to prolonged wound healing times and less than ideal scars. These cure rates range from 70 to 85 percent.
Photodynamic therapy involves the use of a medicine placed on the skin to be preferentially absorbed in pre-cancer or skin cancer cells, where it is metabolized into high levels of a light-sensitive compound that we make at naturally low levels in our body. This resultant chemical then makes the pre-cancer or skin cancer cells very sensitive to bright light—particularly blue or red light. After a calculated incubation period, patients are exposed to a blue or red light, depending on the goal of the therapy (pre-cancer or skin cancer), after which a percentage of the target cells will have been destroyed. This often requires multiple treatments and carries with it some downtime. At times, your dermatologist at Skin Wellness Physicians may recommend combining this method with surgery in order to improve both the surgical experience and cosmetic outcome for your skin cancer treatment.
Topical therapies can be utilized at times, but these treatments often carry the lowest level of success for treating skin cancer. While they may be good options in poor surgical candidates, they often carry with them lengthy treatment protocols and significant skin reactions. However, when used as a pre-treatment to skin cancer surgery, topical therapies can often reduce the extent of the surgery by shrinking the cancer and thus making the procedure less extensive or invasive, with better cosmetic outcomes.
In very rare instances, treatment of skin cancer will require systemic therapies. These are often utilized in very rare circumstances and require a careful and detailed discussion with your dermatologist or oncologist.
At Skin Wellness Physicians, we are committed to maintaining up-to-date treatment options with the most advanced skin cancer treatments and techniques in medical dermatology. As these skin cancer treatments progress, so will our commitment to the best care for you.
How Can You Prevent or Reduce Your Risk of Skin Cancer?
The dermatologists at Skin Wellness Physicians see plenty of patients who develop skin cancer in the Florida sun. While the most common lesions are basal and squamous cell carcinomas, the rarer melanoma is far more aggressive and deadly. With millions of people facing this cancer in the United States, our physicians encourage everyone to practice sun-safe habits to lower the risk and get frequent skin checks to catch suspicious lesions early.
Is skin cancer 100 percent preventable? How can I prevent skin cancer naturally? These are some of the most frequently asked questions we hear about the disease. While no prevention methods are perfect, skin cancer is one of the most preventable diseases. To lower your risk, you will need to take a comprehensive approach to protecting your skin from harmful ultraviolet (UV) radiation. Apply a broad-spectrum sunscreen with an SPF of at least 30 every day. Stay in the shade or limit your sun exposure during the hours when the rays are most intense. Avoid indoor tanning. Wear hats, sunglasses, and other clothing that provides some protection. When skin cancer is detected early, it is highly treatable, so it’s important to see a dermatologist for regular skin checks and examine your own skin for any changes.
When checking your own skin, remember to follow the ABCDEs of skin cancer warning signs. Be sure to note any moles or lesions that have the following characteristics:
A is for Asymmetry: Watch for lesions with two halves that don’t match well.
B is for Border: Keep an eye out for lesions with borders that are indistinct or scalloped.
C is for Color: Lesions that are black, white, blue, or another odd color—or a mix of colors—should be examined.
D is for Diameter: Call out lesions that are larger in diameter than a pencil eraser.
E is for Evolving: Any lesions that is rapidly or noticeable changing in shape, size, color, or general appearance should be cause for concern.
Which Other Medical Treatments Are Available?
We offer many types of medical dermatology treatments at Skin Wellness Physicians, including diagnosis and treatment or management of acne, eczema, rosacea, and psoriasis, as well as numerous other dermatological conditions.
Call (239) 732-0044 or send a message online to arrange a consultation to discuss skin cancer in Naples and Marco Island, FL, at Skin Wellness Physicians.