Navigating Retin A and Retinol: Advice from an Experienced Dermatologist
Retin A is the brand name for prescription topical tretinoin or all-trans retinoic acid, a vitamin A derivative that was first FDA approved in the 1970s for the treatment of acne. Since its introduction, tretinoin has become a first-line agent in the treatment of both acne and photodamage. Retinol, a non-prescription form of retinoic acid, is converted to tretinoin in the body and produces similar beneficial effects but is considered not as strong as its prescription counterpart. Here is what you should know about these powerful options, courtesy of an experienced dermatologist at Florida’s Skin Wellness Physicians.
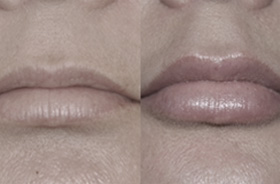
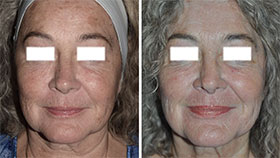
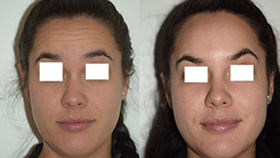
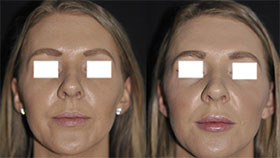
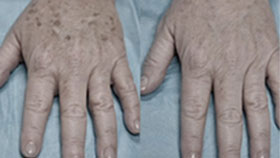
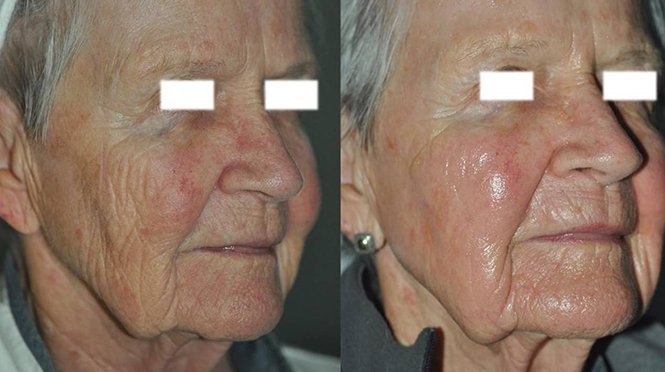
Tretinoin improves acne by binding to specific skin receptors that increase cell turnover and decrease cohesiveness, resulting in exfoliation and reduced follicular plugging. It also reduces sebaceous gland production, decreasing oily skin. In addition, tretinoin promotes collagen formation and reduces pigmentation, making it an effective tool for the treatment of photodamaged skin. Tretinoin is one of the best studied anti-aging ingredients and has multiple double-blind controlled clinical trials that demonstrate improvement of fine wrinkling and brown discoloration.
Despite its multiple benefits, the use of tretinoin cream—and, to a lesser degree, retinol—may be limited by the side effect of skin irritation. Patients with sensitive skin may not tolerate the potential redness, dryness, and flaking it causes. This is especially true at the start of treatment since the side effects tend to lessen as the skin adapts over time. Several strengths and formulations—including creams, gels, and lotions—are available to tailor the product to specific skin types. Newer emollient creams and microencapsulated versions may increase tolerability. Both tretinoin and retinol also cause sun sensitivity and are degraded by sunlight, so should be applied at night followed by routine sunscreen use during the day.
Follow the guidelines below to help minimize tretinoin side effects and obtain the best results:
- At bedtime, wash your face with a gentle cleanser and pat dry. Application of tretinoin to wet skin may increase absorption and hence side effects. Some formulations suggest waiting 15 mins after washing before applying. Remember that other products, such as toners and benzoyl peroxide cleansers, may worsen the dryness so are best stopped altogether or at least delayed until morning.
- Apply a thin layer to your face and avoid sensitive areas such as the corners of the mouth. Avoid eyelids altogether.
- Start slowly. Your dermatologist will likely prescribe a lower concentration of tretinoin at first and may suggest reduced frequency, such as two to three times per week initially. As your skin adjusts with time, gradually increase use to every night at bedtime.
- Moisturize and apply sunscreen with SPF 30 or higher every morning. Applying moisturizer with tretinoin at night helps lessen potential irritation, but also may dilute the concentration.
- Be patient. Acne often looks worse at first and can take two to three months to clear. Expect four to six months to see visible improvement in photodamaged skin.
If you are still unable to tolerate tretinoin, then non-prescription retinol cream may be a better choice. Talk to your dermatologist about a regimen that will best suit your skin type and achieve your goals. Call Skin Wellness Physicians at (239) 732-0044 or submit a contact form to request a consultation.